A Meta-Analysis of Postpartum Copper IUD Continuation Rates in Low- and Middle-Income Countries
Article Information
Angela Marchin1*, Angela Moss2, Margo Harrison2
1Planned Parenthood Federation of America, CO, United States
2University of Colorado School of Medicine, Colorado, United States
*Corresponding author: Margo S Harrison, University of Colorado School of Medicine, Mail Stop B198-2, Academic Office 1, 12631 E. 17th Avenue, Rm 4211, Aurora, Colorado 80045, United States
Received: 04 March 2021; Accepted: 12 March 2021; Published: 18 March 2021
Supplementary File
Citation:
Angela Marchin, Angela Moss, Margo Harrison. A Meta-Analysis of Postpartum Copper IUD Continuation Rates in Low- and Middle-Income Countries. Journal of Women’s Health and Development 4 (2021): 036-046.
View / Download Pdf Share at FacebookAbstract
Background: Long-acting reversible contraception (LARC) initiated immediately postpartum can reduce unintended or mistimed pregnancies, and contribute to proper pregnancy spacing. Data on use and continuation of postpartum LARC in low- and middle-income countries (LMIC) is limited.
Methods: We searched PubMed, OVID, Embase, Google Scholar, Cochrane, POPLINE, Global Health (CABI), and LILACS databases for relevant terms. Studies of any design, published in English, were screened for relevance based on six-month continuation rates of postpartum LARC, location of study, and LARC insertion within 48 hours after vaginal or cesarean birth. We found no relevant studies of implant or hormonal intrauterine device (IUD). Therefore, analysis was limited to studies of the copper IUD only. Two authors used the Cochrane Public Health Group Data Extraction and Assessment Template to guide data extraction to estimate pooled six-month continuation rates, and the Cochrane Risk of Bias Tool for Randomized Controlled Trials and the National Heart, Lung, and Blood Institute (NHLBI) Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies to rate the quality of the studies. A random-effects meta-analysis of proportions was performed.
Results: Immediate-postpartum copper IUDs have a six-month continuation rate of 87% (95% CI 80-92%) in LMIC. The pooled estimated rates of six-month adverse outcomes were 6% (95% CI 5-9%) for expulsion, 5% (95% CI 4-7%) for removal, and 0.2% (95% CI 0.0-0.9%) for infection.
Conclusions: High six-month continuation rates and a low rate of adverse outcomes suggest immediate postpartum copper IUD insertion is a feasible and acceptable postpartum contraceptive option for women living in LMIC.
Keywords
Postpartum
maternal articles maternal Research articles maternal review articles maternal PubMed articles maternal PubMed Central articles maternal 2023 articles maternal 2024 articles maternal Scopus articles maternal impact factor journals maternal Scopus journals maternal PubMed journals maternal medical journals maternal free journals maternal best journals maternal top journals maternal free medical journals maternal famous journals maternal Google Scholar indexed journals neonatal articles neonatal Research articles neonatal review articles neonatal PubMed articles neonatal PubMed Central articles neonatal 2023 articles neonatal 2024 articles neonatal Scopus articles neonatal impact factor journals neonatal Scopus journals neonatal PubMed journals neonatal medical journals neonatal free journals neonatal best journals neonatal top journals neonatal free medical journals neonatal famous journals neonatal Google Scholar indexed journals pregnancies articles pregnancies Research articles pregnancies review articles pregnancies PubMed articles pregnancies PubMed Central articles pregnancies 2023 articles pregnancies 2024 articles pregnancies Scopus articles pregnancies impact factor journals pregnancies Scopus journals pregnancies PubMed journals pregnancies medical journals pregnancies free journals pregnancies best journals pregnancies top journals pregnancies free medical journals pregnancies famous journals pregnancies Google Scholar indexed journals postpartum articles postpartum Research articles postpartum review articles postpartum PubMed articles postpartum PubMed Central articles postpartum 2023 articles postpartum 2024 articles postpartum Scopus articles postpartum impact factor journals postpartum Scopus journals postpartum PubMed journals postpartum medical journals postpartum free journals postpartum best journals postpartum top journals postpartum free medical journals postpartum famous journals postpartum Google Scholar indexed journals meta-analysis articles meta-analysis Research articles meta-analysis review articles meta-analysis PubMed articles meta-analysis PubMed Central articles meta-analysis 2023 articles meta-analysis 2024 articles meta-analysis Scopus articles meta-analysis impact factor journals meta-analysis Scopus journals meta-analysis PubMed journals meta-analysis medical journals meta-analysis free journals meta-analysis best journals meta-analysis top journals meta-analysis free medical journals meta-analysis famous journals meta-analysis Google Scholar indexed journals heterogeneity articles heterogeneity Research articles heterogeneity review articles heterogeneity PubMed articles heterogeneity PubMed Central articles heterogeneity 2023 articles heterogeneity 2024 articles heterogeneity Scopus articles heterogeneity impact factor journals heterogeneity Scopus journals heterogeneity PubMed journals heterogeneity medical journals heterogeneity free journals heterogeneity best journals heterogeneity top journals heterogeneity free medical journals heterogeneity famous journals heterogeneity Google Scholar indexed journals bleeding articles bleeding Research articles bleeding review articles bleeding PubMed articles bleeding PubMed Central articles bleeding 2023 articles bleeding 2024 articles bleeding Scopus articles bleeding impact factor journals bleeding Scopus journals bleeding PubMed journals bleeding medical journals bleeding free journals bleeding best journals bleeding top journals bleeding free medical journals bleeding famous journals bleeding Google Scholar indexed journals mortality articles mortality Research articles mortality review articles mortality PubMed articles mortality PubMed Central articles mortality 2023 articles mortality 2024 articles mortality Scopus articles mortality impact factor journals mortality Scopus journals mortality PubMed journals mortality medical journals mortality free journals mortality best journals mortality top journals mortality free medical journals mortality famous journals mortality Google Scholar indexed journals Heterogeneity articles Heterogeneity Research articles Heterogeneity review articles Heterogeneity PubMed articles Heterogeneity PubMed Central articles Heterogeneity 2023 articles Heterogeneity 2024 articles Heterogeneity Scopus articles Heterogeneity impact factor journals Heterogeneity Scopus journals Heterogeneity PubMed journals Heterogeneity medical journals Heterogeneity free journals Heterogeneity best journals Heterogeneity top journals Heterogeneity free medical journals Heterogeneity famous journals Heterogeneity Google Scholar indexed journals IUD insertion articles IUD insertion Research articles IUD insertion review articles IUD insertion PubMed articles IUD insertion PubMed Central articles IUD insertion 2023 articles IUD insertion 2024 articles IUD insertion Scopus articles IUD insertion impact factor journals IUD insertion Scopus journals IUD insertion PubMed journals IUD insertion medical journals IUD insertion free journals IUD insertion best journals IUD insertion top journals IUD insertion free medical journals IUD insertion famous journals IUD insertion Google Scholar indexed journals
Article Details
1. Background
Use of effective postpartum contraception can lengthen interpregnancy intervals and reduced unintended pregnancy [1]. The World Health Organization (WHO) recommends an interpregnancy interval of at least 24 months in order to minimize maternal and neonatal risks associated with shorter intervals [2]. Short inter-pregnancy intervals are associated with increased risks of preterm birth, maternal morbidities such as anemia, as well as neonatal risks of low birth weight and perinatal death [2]. In a study of Demographic Health Surveys in 21 countries, 61% of postpartum women in LMIC were identified as having an unmet need for family planning, and at least 50% of non-first births occurred in short interpregnancy intervals in nine countries [3].
Initiation of long-acting reversible contraception (LARC), which includes the subdermal implant, and intrauterine devices (IUDs), in the immediate postpartum period, defined as within 48 hours of birth [4], can reduce unintended and/or short-interval pregnancies in a high-income country setting [1]. LARC methods are more effective than short-acting forms of contraception, such as oral contraceptive pills [5]. When LARC methods are offered in an extended postpartum period (up to six weeks after birth) in LMIC, women find it to be an acceptable and appropriate option [6].
In a high-income country setting, twelve-month continuation rates were higher for long-acting methods (86%), including the copper intrauterine device (IUD, 84%), than oral contraceptive pills (55%) and other short-acting methods of contraception [7]. Among women using postpartum family planning in LMIC, 51 to 96% use short-acting methods [3]. This highlights a possible need for increased access to postpartum LARC in LMIC. Given the burden of unintended and short-interval pregnancies in LMIC, and the adverse outcomes associated with these pregnancies, use of postpartum contraception is important [2]. However, there is limited evidence on continuation rates of postpartum LARC methods in LMIC. Continuation rates of contraceptive methods are a proxy indicator of satisfaction [7], and therefore are an important metric to assess when evaluating postpartum LARC initiatives in LMIC. The Family Planning 2020 (FP2020) initiative [8] is a worldwide partnership hosted by the United Nations Foundation that assists 69 committed low-income countries in improving access to contraceptives and helps women achieve their reproductive goals [8]. This initiative has also works to improve data collection and availability in these countries. A stated goal of FP2020 is to “work toward increasing the availability, visibility, quality, and use of family planning data.”
Therefore, the objective of this systematic review and meta-analysis was to determine six-month continuation rates of LARCs inserted within 48 hours of birth in countries involved in the FP2020 initiative [8]. As we found zero relevant studies on other LARC methods, we ultimately focused on the copper IUD that is currently available, the CuT380A. We hypothesized that the six-month continuation rate would be comparable to those in high-income countries, which is over 80% [7]. Secondary aims included determining six-month IUD removal, expulsion, pain, bleeding, infection, pregnancy, and missing string rates.
2. Methods
2.1 Search strategy
In August 2017, we searched PubMed, OVID, Embase, Google Scholar, Cochrane, POPLINE, Global Health (CABI), and LILACS for search terms and MESH terms (PubMed) developed by the senior author (MSH) and a clinical librarian. We did not use any specialized search software. The search terms included all synonyms and related terms to the following key concepts: (1) “postpartum,” (2) “LMIC,” (3) FP2020 countries, (4) “LARC,” and individual LARC types and (5) “continuation rate.” Search formatting was adjusted to fit the interface requirements of each database. No hand searching was performed. See Appendix A for full search strategy.
2.2 Inclusion criteria
Studies of any design published in English were considered. The first author (ALM) and MSH screened abstracts for relevance based on publication of six-month continuation rates, location of the study in one of the FP2020 countries [8] (see Appendix B) and insertion of the LARC method either “post-placentally” (within 10 minutes of expulsion of placenta) or “immediately postpartum” (within 48 hours) after vaginal or cesarean deliveries. We focused on this time-period because this is how FP2020 and the WHO define care provided in the “pre-discharge” stage of perinatal care [4]. Included countries were limited to those in the FP2020 initiative to improve the relevance of results, given that these countries are committed to postpartum contraceptive initiatives [8]. After all relevant abstracts were identified, inclusion criteria were then refined to include only copper IUDs when scant to no evidence for other LARC methods (implant or other types of IUDs) was identified. When a citation yielded only an abstract, we attempted to contact a corresponding author electronically to inquire whether a subsequent article had been published based on the abstract data, or if unpublished manuscripts could be shared. ALM and MSH then performed full text screening to confirm studies met all inclusion criteria. A flow diagram of determinations regarding the reviewed abstracts and manuscripts are shown in Figure 1.
2.3 Quality determination
Authors ALM and MSH independently rated the quality of evidence in each study based on the Cochrane Risk of Bias Tool for Randomized Controlled Trials [9] and the National Heart, Lung, and Blood Institute (NHLBI) Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies [10]; these authors then met to discuss and resolve discrepancies. Studies of fair quality or better were included.
2.4 Data extraction
We used the Cochrane Public Health Group Data Extraction and Assessment Template [11] to guide extraction of relevant data. Authors ALM and MSH extracted data separately and met to discuss and resolve discrepancies.
2.5 Data analysis
Data was analyzed with R software and the meta [12] and metaphor [13] packages. All statistical tests were performed with p<0.05 significance. To estimate pooled six-month continuation rates, a random-effects meta-analysis of proportions was performed. The logit transform was performed which is recommended when the observed proportions are >0.8 [14]. The DerSimonian and Laird [15] method was used to estimate between-study variance. Heterogeneity was assessed with Tau2, I2 and the Q-test. A forest plot was created to visualize the point estimates of the studies and their confidence intervals. Studentized residuals were screened to identify potential outlier studies (abs value Z>2.0). To determine the influence of outliers on model results, a “leave one out” analysis was performed. Modifiers were assessed as possible sources of heterogeneity with subgroup analysis. Subgroup analysis of country as a modifier was done assuming a common variance between-study component (or pooled tau2). Summary effects of each subgroup were compared with a mixed effect model. Secondary six-month outcome rates of expulsion, removal, bleeding, missing strings, and infection were pooled with a random effects meta-analysis. Double arcsine transformation was used for the rare outcome of infection. Otherwise, proportions were transformed with the logit transformation. Forest plots were created for each secondary outcome.
2.6 Ethics approval
As we used aggregated, de-identified data from other
studies in which human subjects approval was obtained, we did not seek approval from an institutional review board or obtain consent from subjects.
3. Results
3.1 Study selection
The search strategy yielded 481 abstracts after duplicates were removed. After abstract screening was completed, 108 full-text studies were assessed for eligibility, and 11 studies [16-26] were included. See Figure 1 for screening flow diagram and reasons for exclusion. For the purposes of data analysis, one study [26] was divided into two as it took place in two different countries and presented separate data for each. Table 1 lists study details.
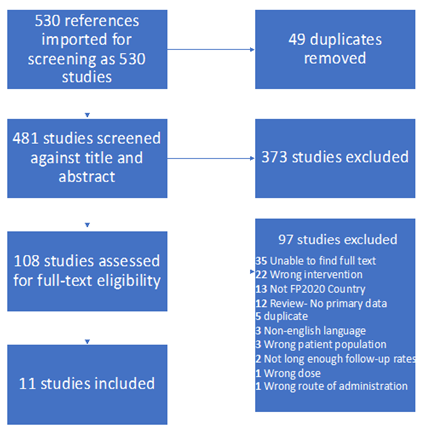
Figure 1: Screening flow diagram.
*Quality of evidence determined by the Cochrane Risk of Bias Tool for Randomized Controlled Trials and the National Heart, Lunch, and Blood Institute (NHLBI) Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies
Table 1: Study characteristics.
3.2 Description of studies
Of the 11 included studies, nine [16-23, 26] were prospective cohorts and two [24, 25] were randomized controlled trials. Six of the prospective cohorts [16, 17, 19-21] compared outcomes after post-placental (within ten minutes) copper IUD insertion between women delivering vaginally and via cesarean. Two prospective cohort study [22, 26] compared outcomes between post-placental insertion and later insertion (within 48 hours of delivery [22]or within 72 hours [26]; in women delivering vaginally or via cesarean. In the cohort that compared post-placenta insertion vs insertion up to 72 hours, only the data from the post-placental insertion group was used in analysis, as 72 hours was outside of the window for our inclusion criteria. One prospective cohort [18]recorded outcomes of post-placental insertion of copper IUDs in women undergoing cesarean deliveries only. Another prospective cohort [23] recorded outcomes after IUD insertion within 48 hours of vaginal delivery only. One randomized controlled trial (RCT) compared outcomes between two different types of copper IUDs among women delivering vaginally; data from only the copper 380A IUD was used in our analysis [24].The other RCT compared outcomes between post-placental insertion and delayed (>6 weeks) insertion; only data from post-placental insertion participants was used for our analysis [25].
3.3 Quality assessment
After initial independent quality assessment, MSH and ALM had two overall quality score discrepancies that were resolved through review and discussion. Ultimately, five studies were determined to be of good quality and six were of fair quality.
3.4 Primary outcome
The meta-analysis of all 12 studies (11 studies with
Morrison, et al [26] considered as two) resulted in a
pooled six-month continuation rate of 87% (0.87, 95% CI 0.80,0.92) (Figure 2). However, there is a significant (Q-test p= <0.0001) amount of heterogeneity (tau2 = 0.76) which was mostly between studies (I2 = 97%). The Mishra 2014 study was indicated as an outlier (abs z = 2.13). Removing this study resulted in less heterogeneity (tau2 = 0.45). However, this had little effect on the pooled proportion and confidence interval estimates (0.88, 95% CI 0.83,0.92). Therefore, no studies were removed as outliers in this analysis. Country (India vs other) was examined in moderator subgroup analysis to determine if it explained a significant amount of the heterogeneity of studies for six-month continuation rates because 7 of the 12 studies were executed in India. The pooled six-month continuation rates in the India studies did not differ significantly from that of studies from other countries (0.87, 95% CI 0.76,0.93] vs 0.87, 95% CI 0.74,0.94; p = 0.89).
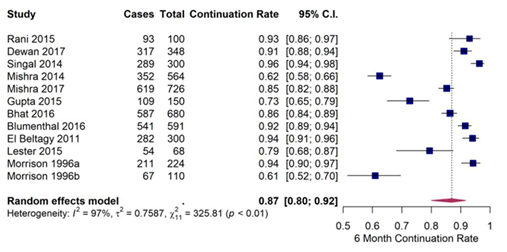
Figure 2: Forest Plot of Continuation Rates.
3.5 Secondary outcomes
The pooled estimated expulsion rate across all studies was 6% (0.06, 95%CI 0.05,0.09). The pooled removal rate for the 11 studies that included removal data was 5% (0.05, 95% CI 0.04,0.07). The pooled rate of bleeding at six months was 22% (0.22, 95% CI 0.07,0.52) for the six studies that had bleeding data. However, one study stood out on the forest plot with a bleeding proportion of 89%. Seven studies had data on six-month missing string rates; the pooled proportion for those missing strings at six months was 17% (0.17, 95% CI 0.11,0.27). Four of the eight studies with infection data indicated no infection occurred. The pooled proportion for six-month infection was 0.2% (0.002, 95% CI 0.000,0.009).
4. Conclusions
This is the first meta-analysis, to our knowledge, of immediate postpartum copper IUD continuation rates in LMIC. Our finding of a six-month continuation rate of 87% is important to global public health because this rate is comparable to continuation rates found in higher-income countries [7]. This estimate did, however, have significant heterogeneity between studies. Secondary outcomes of expulsion, removal, and infection rates were low at 6%, 5%, and 0.2% respectively. This analysis has generalizability because the quality assessment performed on the studies included used validated quality assessment tools, and all the of studies were of fair or better quality. Studies that were excluded would not have been able to contribute to the primary outcome so we do not think the sample is biased by their exclusion. Additionally, as this was unfunded study, we were unable to translate non-English language manuscripts, of which there three; we did not use internet-based translating tools because the files of the manuscripts were images and not selectable text.
The results of this meta-analysis are important for future efforts to increase access to postpartum copper IUDs in LMIC. In a study of acceptability of post-partum IUDs among women in Nigeria, 50% of those who were offered a postpartum IUD accepted this method [27]. Since continuation rates can reflect satisfaction with a contraceptive method [7], our results add to the evidence that immediate postpartum copper IUD is acceptable to women in LMIC, and that women are likely to be very satisfied with this method. Notably, rates of complications, such as infection and expulsion, were low and consistent with data from higher-income countries [28-31]. These findings can be used to support programs that increase accessibility to postpartum copper IUD insertion in LMIC. Immediate postpartum copper IUD insertion has promise for improving birth spacing, unmet need for family planning, and resulting maternal, child, and neonatal morbidity and mortality [2]. When interpreting these results, it is important to consider alternative explanations for the high continuation rates. Specifically, in LMIC, it may be difficult for women to present to a care provider to have their IUD removed if they so desire [32]. However, the majority of these studies had little loss-to-follow-up, suggesting that these patients had adequate access to care. Another possible explanation for high continuation rates is provider coercion, which has been a global concern with contraception and sterilization among poor or otherwise marginalized people [33]. However, the studies included in this review reported following ethical research practices, including antenatal contraceptive counseling, and obtaining informed consent. Our focus on FP2020-committed countries can also provide reassurance that coercion is less likely, due to the initiative’s focus on rights-based family planning programs; specifically, FP2020 initiatives aim to provide family planning services that aim to improve agency and autonomy, and prevent coercion [8].
The main strength of this study is that it is a novel investigation to summarize what is known about continuation rates of copper IUDs inserted postpartum in LMIC. Additionally, all data included in the meta-analysis were from published studies of fair or better quality. Additionally, collaborating with a librarian allowed for rational search strategy and identification of a comprehensive cohort of high-quality studies to screen and analyze. A weakness of the study is the heterogeneity identified between studies. This was reduced when one potential outlier was removed, but this did not have a significant impact on the meta-analytic estimate of the six-month continuation rate. This heterogeneity could possibly be explained by differences between the six countries included in the study and in different timing of IUD insertion between studies. However, the potential outlier study was executed in India, where five other studies were also performed. Other limitations of this review are that included data was only from studies published in English from six countries, which limits our ability to generalize to more LMIC.
Another significant finding discovered during the systematic review was the extremely limited evidence on postpartum use of other LARC methods such as the levonorgestrel IUD and the progestin-containing implants. This may reflect cost differences, access or availability, and/or patient preferences, but more studies are needed to identify the feasibility of offering these additional methods in the immediate postpartum period in LMIC. Our findings can be used to educate providers about the public health relevance of immediate postpartum IUD initiation. Future knowledge, attitudes, and practice assessments of health care providers in LMIC will help with directing program implementation efforts to improve delivery and accessibility of postpartum IUD. It is also not known how often immediate postpartum IUD is being offered in LMIC. In regions where little is known about postpartum contraception, needs assessments and qualitative studies exploring patient and provider values may be considered for next steps in exploring postpartum IUD program implementation.
Acknowledgements
We wish to acknowledge our clinical librarian, Kristen DeSanto, MSLS, MS, RD, AHIP, for her assistance in formulating our search strategy. This work was supported by the Eunice Kennedy Shriver National Institutes of Child Health and Human Development Women’s Reproductive Health Research K12 award (5K12HD001271-18) and the Doris Duke Charitable Foundation.
Funding
Funding for this project comes from the Eunice Kennedy Shriver National Institute of Child Health and Human Development Women’s Reproductive Health Research K12 award (5K12HD001271-18) and the Doris Duke Charitable Foundation.
Conflict of Interest
The authors have no relationships to disclose that may be deemed to influence the objectivity of this paper and its review. The authors report no commercial associations, either directly or through immediate family, in areas such as expert testimony, consulting, honoraria, stock holdings, equity interest, ownership, patent-licensing situations or employment that might pose a conflict of interest to this analysis. Additionally, the authors have no conflicts such as personal relationships or academic competition to disclose. The findings presented in this paper represent the views of the named authors only, and not the views of their institutions or organizations.
References
- White K, Teal SB, Potter JE. Contraception after delivery and short interpregnancy intervals among women in the United States. Obstet Gynecol 125 (2015): 1471-1477.
- World Health Organization (WHO). Report of a technical consultation on birth spacing, Geneva Switzerland, 13–15 June 2005. Geneva: World Health Organization (2007).
- Moore Z, Pfitzer A, Gubin R, et al. Missed opportunities for family planning: an analysis of pregnancy risk and contraceptive method use among postpartum women in 21 low- and middle-income countries. Contraception 92 (2015): 31-39.
- World Health Organization (WHO). Programming strategies for postpartum family planning. Geneva, Switzerland: World Health Organization (2013)
- World Health Organization Department of Reproductive Health and Research (WHO/RHR) and Johns Hopkins Bloomberg School of Public Health/Center for Communication Programs (CCP), Knowledge for Health Project. Family Planning: A Global Handbook for Providers (2018 update). Baltimore and Geneva: CCP and WHO (2018).
- Vernon R. Meeting the Family Planning Needs of Postpartum Women. Studies in Family Planning 40 (2009): 235-245.
- Peipert JF, Zhao Q, Allsworth JE, et al. Continuation and Satisfaction of Reversible Contraception. Obstetrics & Gynecology 117 (2011): 1105-1113.
- Family Planning FP 2020. FP 2020 69 Focus Countries. Family Planning 2020 website (2018).
- The Cochrane Public Health Group. Data Extraction and Assessment Template. Cochrane Training website (2011).
- The Cochrane Collaboration. Cochrane Risk of Bias Tool for Randomized Controlled Trials. The Cochrane Collaboration website (2011).
- National Heart, Lung, and Blood Institute. Quality Assessment Tool for Observational Cohort and Cross-Sectional Studies. National Heart, Lung, and Blood Institute website (2018).
- Schwarzer G, Carpenter JR, Rücker G. Meta-Analysis With R. Cham, Switzerland: Springer (2015).
- Viechtbauer W. Conducting Meta-Analyses in R with the metafor Package. Journal of Statistical Software 36 (2010): 1-48.
- Wang Naike. How to Conduct a Meta-Analysis of Proportions in R: A Comprehensive Tutorial (2018).
- DerSimonian R, Laird N. Meta-analysis in clinical trials. Controlled clinical trials 7 (1986): 177-188.
- Rani M, Kaur P, Kaur K, et al. A study of clinical outcomes of postpartum intrauterine contraceptive device. Journal of Family Welfare 61 (2015): 32-38.
- Dewan R, Dewan A, Singal S, et al. Non-visualisation of strings after postplacental insertion of Copper-T 380A intrauterine device. Journal of Family Planning and Reproductive Health Care 43 (2017): 186-1941-1949.
- Singal S, Bharti R, Dewan R, et al. Clinical Outcome of Postplacental Copper T 380A Insertion in Women Delivering by Caesarean Section. Journal of Clinical and Diagnostic Research 8 (2014): OC01-OC04.
- Mishra S. Evaluation of Safety, Efficacy, and Expulsion of Post-Placental and Intra-Cesarean Insertion of Intrauterine Contaceptive Devices (PPIUCD). The Journal of Obstetrics and Gynecology of India 64 (2014): 337-343.
- Mishra S. Tale of the Tails, the Missing Postpartum IUCD Strings. The Journal of Obstetrics and Gynecology of India 67 (2017): 202-207.
- Gupta G, Goyal R, Kadam VK, et al. The Clinical Outcome of Post Placental Copper-T-380A Insertion with Long Placental Forceps (Kelly’s Forceps) After Normal Vaginal Delivery and Cesarean Section. The Journal of Obstetrics and Gynecology of India 65 (2015): 386-388.
- Bhat SS, Damle H, Darawade SP, et al. To study the acceptance of postpartum intrauterine contraceptive device, CU T 380 A, in a tertiary care hospital in India. Journal of Reproductive Health and Medicine 2 (2016): 93-98.
- Blumenthal PD, Chakraborty NM, Prager S, et al. Programmatic experience of post-partum IUD use in Zambia: an observational study on continuation and satisfaction. The European Journal of Contraception & Reproductive Health Care 21 (2016): 356-360.
- El Beltagy NS, Darwish EA, Kasem MS, et al. Comparison between Cupper T380 IUD and Multiload 375 in early post partum insertion. Middle East Fertility Society Journal 16 (2011): 143-148.
- Lester F, Kakaire O, Byamugisha J, et al. Intracesarean insertion of the Copper T380A versus 6 weeks postcesarean: a randomized clinical trial. Contraception 91 (2015): 198-203.
- Morrison C, Waszak C, Katz K, et al. Clinical outcomes of two early postpartum IUD insertion programs in Africa. Contraception 53 (1996): 17-21
- Sodje 2016.
- Dahlke JD, Terpstra ER, Ramseyer AM, et al. Postpartum insertion of levonorgestrel–intrauterine system at three time periods: a prospective randomized pilot study. Contraception 84 (2011): 244-248.
- Hayes JL, Cwiak C, Goedken P, et al. A pilot clinical trial of ultrasound-guided postplacental insertion of a levonorgestrel intrauterine device. Contraception 76 (2007): 292-296.
- Celen S, Sucak A, Yildiz Y, et al. Immediate postplacental insertion of an intrauterine contraceptive device during cesarean section. Contraception 84 (2011): 240-243.
- Welkovic S, Costa LO, Faundes A, et al. Post-partum bleeding and infection after post-placental IUD insertion. Contraception 63 (2001): 155-158.
- Joint WHO/World Bank Group report. Tracking universal health coverage: First global monitoring report. Geneva: World Health Organization (2015).
- Guttmacher policy review Summer 2014, Rachel Benson Gold. Guarding Against Coercion While Ensuring Access: A Delicate Balance (2014).


 Impact Factor: * 1.1
Impact Factor: * 1.1 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 