Analgesic Effect of Continuous Rate Infusion of Butorphanol in Unilateral Total Resection of Mammary Tumor in Dogs
Article Information
Kenichi Maeda*, Honoka Nomura, Daiki Hotta, Takuma Matsui, Satomi Iwai, Shozo Okano
Laboratory of Small Animal Surgery 2, School of Veterinary Medicine, Kitasato University, Towada, Aomori, Japan
*Corresponding Author: Kenichi Maeda, Kitasato University School of Veterinary Medicine, Small Animal Surgery 2, Kenichi Maeda, Japan
Received: 24 January 2020; Accepted: 03 February 2020; Published: 05 February 2020
Citation: Kenichi Maeda, Honoka Nomura, Daisuke Hotta, Takuma Matsui, Satomi Iwai, Shozo Okano. Analgesic Effect of Continuous Rate Infusion of Butorphanol in Unilateral Total Resection of Mammary Tumor in Dogs. Archives of Veterinary Science and Medicine 3 (2020): 22-30.
View / Download Pdf Share at FacebookAbstract
Unilateral resection of mammary gland tumor (MGT) induce severe pain and it is necessary to use narcotic analgesics. Butorphanol has a weak analgesic effect and is effective for moderate pain, but it is thought that effective analgesia can be obtained by combining with other analgesics. However, since the information of analgesic effect of butorphanol is limited, this study compared the analgesic effect of continuous rate infusion (CRI) of butorphanol with fentanyl, a narcotic opioid, in MGT unilateral resection. 14 dogs undergoing MGT unilateral resection at Kitasato University Veterinary Teaching Hospital were randomly assigned to the fentanyl administration group (F group, n=8) and the butorphanol administration group (Group B, n=6). All patients were induced anesthesia by propofol and maintained with isoflurane. In group F, fentanyl(0.005 mg/kg) was injected followed by CRI (0.005 to0.02 mg/kg/hr). In group B, after injected initial dose of butorphanol (0.1 mg/kg), CRI was started (0.2 to 0.4 mg/kg/hr). Bupivacaine (1 mg/kg) was infiltrated into the wound surface after tumor removal, and CRI was discontinued at the start of wound closure, and buprenorphine was IV. Heart rate and inhalational anesthesia concentration were recorded during anesthesia and the pain score was evaluated after recovered from anesthesia. There was no significant difference in heart rate, inhalation anesthetic concentration and the pain score between the two groups. It was found that analgesia with butorphanol was effective as same as fentanyl when combined with other analgesics. These results will provide choices of analgesic protocols for several surgical procedures.
Keywords
Analgesia; Butorphanol; Buprenorphine; Mammary gland tumor
Analgesia articles, Butorphanol articles, Buprenorphine articles, Mammary gland tumor articles
Article Details
1. Introduction
Pain management is crucial element because perioperative pain affects surgical outcomes. Although there are various analgesics used in the perioperative period, opioids have a strong analgesic effect by binding to three types of receptors, μ, δ, and κat various sites such as the dorsal horn of the spinal cord and the cerebrum. Therefore, it is considered to be the main axis of analgesia in the perioperative period. However, although it has high analgesic effects, it is known that mu receptor agonists may cause respiratory depression and gastrointestinal dysfunction as side effects, and caution is required when using high doses [1 , 2]. In order to reduce the risk of such side effects, multimodal analgesia, which combines multiple analgesics with different mechanisms of action other than opioids, as a method of obtaining an appropriate analgesic effect while suppressing the dose of opioids, has been recommended [3, 4]. In addition, morphine and fentanyl, which have strong analgesic effects, are designated as narcotics, and their use is severely restricted in some countries and regions, and may not be suitable for daily use. Butorphanol is a non-narcotic opioid and an analgesic widely used in clinical practice.
Butorphanol acts as a partial antagonist for μ receptor and shows an analgesic effect mainly by binding to κ receptor [5]. Compared with narcotic μ receptor agonist, it has less respiratory depression effect and is used. It is an easy drug. However, its analgesic effect is relatively weak and has a ceiling effect, so it is considered to be effective up to moderate pain, making it unsuitable for analgesia in highly invasive surgery. Its analgesic effect is relatively short and requires frequent or continuous administration. The analgesic effects of continuous intravenous butorphanol administration in the perioperative period are occasionally seen in horses [6] and cattle [7], but there are no reports on dogs as far as authors know. Unilateral total resection of the mammary tumor (MGT) in dogs is a routine surgical procedure performed in clinical settings. Since the mammary gland extends from near the arm pits to the groin, the incision to remove the tumor reaches almost the entire length of the trunk, and the size of the incision indicates that the degree of intraoperative pain is moderate or higher. For this reason, our university animal hospital uses fentanyl, a narcotic opioid, as an analgesic. Therefore, in this study, we evaluated the analgesic effect of continuous intravenous administration of Butorphanol with MGT unilateral total resection in dogs using a drug with few restrictions in clinical practice to establish an analgesic method without using narcotic opioids.
2. Material and Methods
2.1 Experimental animal
After the approval of the Kitasato University Animal Experiment Committee and the owner's approval, 14 dogs undergoing unilateral total MGT resection at the Kitasato University Animal Hospital. Age and weight were recorded in all animals, fasted 6 hours before induction of anesthesia, and stopped watering 2 hours before anesthesia.
2.2 Group setting
A group receiving fentanyl as an intraoperative analgesic (Group F, n=8) and a group receiving butorphanol (Group B, n=6) were set, and 14 dogs were randomly assigned into two groups.
2.3 Induction and maintenance of anesthesia
22G indwelling needle (Surflow Flash®22G × 1: Terumo; Tokyo, Japan) was placed in the cephalic vein of all animals. The infusion was performed using Ringer's lactate solution (Lactec® : Otsuka Pharmaceutical; Tokyo, Japan) at 5 ml/ kg /hr during surgery and 3 ml/ kg /hr after surgery. All animals receive 0.2 mg/kg of meloxicam (Metacam® 0.5% Injection: Boehringer Ingelheim Animal Health Japan; Tokyo, Japan) subcutaneously before surgery, and midazolam (Dormicum® Injection 10 mg: Astellas Pharmaceutical) as premedication ; Tokyo, Japan) 0.1 mg/kg was administered intravenously. Then, in group F, fentanyl (Fentanyl Injection®: Daiichi Sankyo; Tokyo, Japan) 0.005 mg/kg intravenously and continuous intravenous administration was started at 0.005-0.02 mg/kg/hr. In group B, 0.1 mg/kg of butorphanol (Vetorphale ®: Meiji Seika Pharma; Tokyo, Japan) was administered intravenously, and continuous intravenous administration was started at 0.2 to 0.4 mg/kg/hr. For anesthesia induction, propofol (1% propofol injection “Maruishi”: Maruishi Pharmaceutical; Osaka, Japan) was intravenously administered to both groups until endotracheal intubation was possible with To Effect, and then isoflurane (animal isoflurane: MSD animal Health; Tokyo, Japan) Anesthesia was maintained at 1.5-2.5%. The respiratory rate, airway pressure and inspiratory expiration ratio are controlled using a ventilator (Animal artificial respiration system KVS-2100: Koken Medical; Tokyo, Japan) and ECG, blood oxygen saturation (SPO?), end-tidal carbon dioxide concentration (ETCO?), Isoflurane concentration , blood pressure was measured by using a biological information monitor (animal biological information monitor BP-608; Fukuda Colin, Tokyo). The operation was performed based on the general procedure of unilateral MGT total resection. After excision of the tumor, the wound surface was infiltrated with 1 mg/kg of bupivacaine (Marcaine® 0.5%: Aspen Japan; Tokyo, Japan), and then subcutaneous suture was performed. At the start of skin suture, continuous intravenous administration was stopped in both groups, and 0.02 mg/kg of buprenorphine (Lepetan® injection 0.2 mg; Otsuka Pharmaceutical; Tokyo, Japan) was administered intravenously. The surgical time from incision to wound closure was recorded in all animals, and the heart rate and inhalation anesthesia concentration every 10 minutes during the operation were recorded.
2.4 Pain score
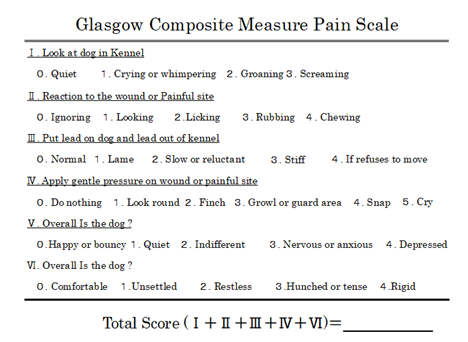
Pain score was evaluated every 30 minutes from 0 minutes after anesthesia recovering until 2 hours thereafter. The evaluation was performed for the following six items based on the Glasgow complex pain scale shown below, and the total value was used as a score at each time point (Figure 1).
2.5 Statistical analysis
Statistical software JMP (SAS?Cary, North Carolina, U.S.A) was used for statistical analysis. Student's t-test was used to compare age, weight, operative time, and intraoperative heart rate and inhalation anesthesia concentration between the two groups. In addition, a Wilcoxon rank sum test was used for the comparison of pain scores between the two groups, and a Wilcoxon signed rank sum test was used for the intragroup comparison. p <0.05 was considered significant difference.
3. Results
3.1 Age
The age of the two groups was 9.62 ± 2.05 years in the F group and 9 ± 1.52 years in the B group, and no significant difference was observed (Table 1).
3.2 Body weight
The weight of the two groups was 8.37 ± 5.32 kg in the F group and 5.29 ± 3.79 kg in the B group, and no significant difference was observed (Table 1).
3.3 Duration of anesthesia time
The duration of anesthesia time of the two groups was 84.62 ± 27.43 minutes in group F and 79.16 ± 23.96 minutes in group B, and no significant difference was observed (Table 1).
|
Group F |
Group B |
|
|
Age (Year) |
9.62 ± 2.05 |
9.00 ± 1.52 |
|
Body Weight (Kg) |
8.37 ± 5.32 |
5.29 ± 3.79 |
|
Duration of anesthesia (min) |
84.62 ± 27.43 |
79.16 ± 23.96 |
Table 1: The age, body weight and duration of anesthesia of group F and group B were shown. No significant difference was observed between the groups each subject.
3.4 Intraoperative heart rate
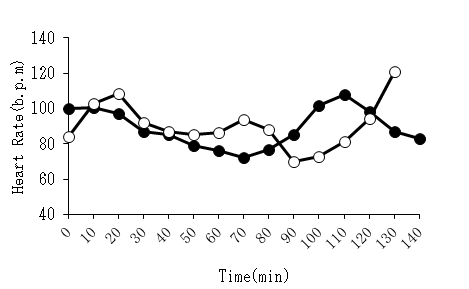
(Figure 2) Shows the changes in heart rate during the operation. No significant difference was observed between groups at any time point.
3.5 Intraoperative inhalation anesthesia concentration
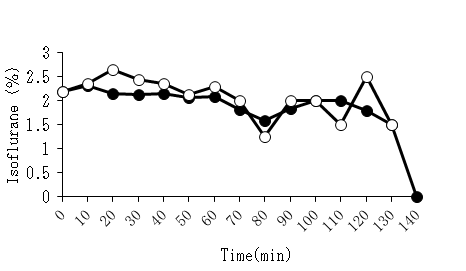
(Figure 3) Shows the changes in the inhalation anesthesia concentration during the operation. No significant difference was observed between groups at any time point.
3.6 Pain score
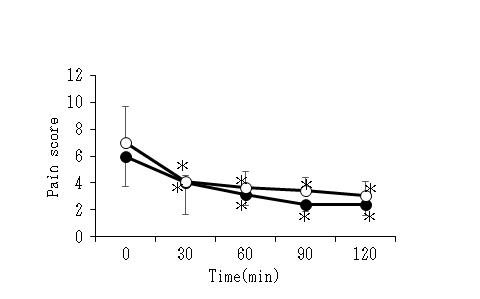
The transition of the average value of the pain scores of the two groups is shown in (Figure 4). The score was 6 ± 2.27 in the F group and 7 ± 2.69 in the B group at 0 minutes after recovering, and both groups showed the maximum value. After 30 minutes, the value was 4.06 ± 2.39 in the F group and 4.08 ± 0.44 in the B group, and the values were significantly reduced in both groups. Thereafter, it gradually decreased with time, and after 120 minutes, it was 2.37 ± 0.78 in the F group and 3.08 ± 1.05 in the B group. The score tended to be higher in the B group than in the F group throughout the measurement period, but no significant difference was observed between the groups at any time.
Figure 4: The changes in pain scores after the operation in the F group and the B group were shown. After the waking of the anesthesia, the scores of both groups were significantly reduced, and were lower than those at the time of waking throughout the measurement period. The scores tended to be lower in the F group than in the B group, but no significant difference was observed between the two groups. (Group F : white circle, Group B : black circle, ??P < 0.05).
4. Discussion
The non-narcotic opioid butorphanol is an analgesic that mainly acts on the kappa receptor and partially on the μ receptor [8]. Compared to the strong opioid fentanyl, which has a high affinity for the μ receptor, butorphanol is not enough as an analgesic in MGT unilateral total resection in which the analgesic effect is weak, moderate or higher, and severe pain is expected it is conceivable that. Because fentanyl has good blood regulation, pain management is performed by continuous intravenous administration during surgery, but butorphanol also requires a short blood half-life and continuous intravenous administration. Fentanyl is usually administered intravenously in the range of 5 to 30 µg/kg/hr, but if the patient is severely painful, increasing the rate of administration can provide stronger analgesia. On the other hand, butorphanol is administered in the range of 0.1 to 0.4 mg/kg/hr, but because of the ceiling effect, if the patient feels pain, increasing the administration rate does not enhance the analgesic effect. In such a case, it is necessary to expect the effects of other anesthetic analgesics such as temporarily increasing the concentration of the inhaled anesthetic. In this study, the degree of pain in the patient during surgery was evaluated by the increase in heart rate due to the sympathetic reflex. Intraoperative concentrations of inhalational anesthetics were compared, and the isoflurane use concentration of the butorphanol use group was compared with that of the fentanyl group. There was no significant difference in heart rate between the fentanyl group and the butorphanol group. Also, there was no difference between the two groups in the concentration of isoflurane, and it was considered that it was not necessary to increase the amount of isoflurane in the butorphanol administration group compared to the fentanyl administration group. Therefore, it is considered that the intraoperative analgesic effect of unilateral total resection of the mammary gland could be managed by continuous intravenous administration of butorphanol as well as by continuous intravenous administration of fentanyl.
If fentanyl is administered for postoperative analgesia after awakening of anesthesia, respiratory depression may occur. For this reason, when administering fentanyl even after surgery, it is necessary to monitor the patient's respiratory condition during the administration period, which is not a practical method in a private practice where the number of personnel is limited. Buprenorphine, as same as fentanyl, is a μ receptor agonist and has a strong analgesic effect, butorphanol has a ceiling effect and is unlikely to cause side effects such as respiratory depression [9, 10]. In addition, because of its high liposolubility and strong affinity with the receptor, a single intravenous or intramuscular administration can provide an analgesic effect over a long period of 6 hours or more [9]. Therefore, by administering buprenorphine at the end of continuous intravenous administration of fentanyl, it becomes possible to reduce the risk of respiratory depression and perform postoperative pain management. Butorphanol, like buprenorphine, has a ceiling effect on its receptors, and the risk of respiratory depression is low even when administered after awakening of anesthesia [11]. However, butorphanol, like fentanyl, has a relatively short blood half-life, so frequent or continuous administration is required to maintain effective blood levels. Therefore, it is considered that continuous intravenous administration of butorphanol is stopped after surgery, and administration of buprenorphine can provide an analgesic effect for a long time with a single administration, thereby facilitating postoperative management. However, it is known that butorphanol and buprenorphine antagonize at the μ receptor, and since buprenorphine is also a κ receptor antagonist, it has been reported that the analgesic effect is diminished by using these drugs in combination [12]. In this study, it is possible that antagonism between butorphanol and buprenorphine might occur, and it was also predicted that postoperative pain scores would increase. However, as in the fentanyl group, the pain score of the butorphanol group declined with the passage of time after anesthesia was awake, and there were no individuals whose analgesic effect was antagonized and pain was exacerbated. Probably did not occur.
Jhonson et al. report that administering butorphanol and buprenorphine simultaneously in cats did not produce effective analgesic effects and there was no merit in combination [12]. In this study, buprenorphine was not given at the same time as butorphanol, but was given at a certain time after the end of continuous intravenous administration, at which time the But disappeared from the blood. Therefore, it is considered that the analgesic effect of butorphanol overlapped in the process of decreasing the blood concentration of butorphanol. However, this study did not measure the blood concentration of butorphanol, and there are no reports to date on the evaluation of the blood concentration of butorphanol in the case of continuous intravenous administration. Therefore, in this study, it was not possible to confirm the disappearance of butorphanol from the blood, and it was not possible to confirm the relationship with the increase in the blood concentration of buprenorphine. In conclusion, it was found that multimodal analgesia, continuous intravenous administration of butorphanol combining NSAIDs and local anesthetics provide equivalent an analgesic effect to that of fentanyl by in MGT unilateral total resection of dogs. It was also confirmed that it is possible to manage pain by administering buprenorphine after surgery using butorphanol. Therefore, butorphanol multi modal pain management may be a viable option when performing surgery in facilities where drugs are not available or where staffing is limited. However, the degree of pain of the MGT unilateral total resection in this study was not so sever than that of thoracotomy or amputation, and narcotic opioids and NMDA receptor antagonist should be needed for these surgeries.
Conflict of Interest
There is no conflict of interest in this article. Thank you for your peer review.
References
- Greer JJ, Carter JE, al-Zubaidy Z.Opioid depression of respiration in neonatal rat. J Physiol 485 (1995): 845-855.
- Takita K, Herlenius EA, Lindahl SG, et al. Actions of opioids on respiratory activity via activation of brainstem mu-, delta- and kappa-receptors; an in vitro study.Brain Res 778 (1997): 233-241.
- Gritsenko K, Khelemsky Y, Kaye AD, et al. Multimodal therapy in perioperative analgesia.Best Pract Res Clin Anaesthesiol 28 (2014): 59-79.
- Wick EC, Grant MC, Wu CL. Postoperative Multimodal Analgesia Pain Management With Non opioid Analgesics and Techniques.JAMA Surg 152 (2017): 691-697.
- Walsh SL, Chausmer AE, Strain EC, et al. Evaluation of the Mu and Kappa Opioid Actions of Butorphanol in Humans Through Differential Naltrexone Blockade. Psychopharmacology(Berl) 196 (2008): 143-155.
- Sanz MG, Sellon DC, Cary JA, et al. Analgesic effects of butorphanol tartrate and phenylbutazone administered alone and in combination in young horses undergoing routinecastration.J Am Vet Med Assoc 235 (2009): 1194-1203.
- Baldridge SL, Coetzee JF, Dritz SS, et al. Pharmacokinetics and physiologic effects of intra-muscularly administered xylazine hydrochloride-ketamine hydrochloride-butorphanol tartrate alone or in combination with orally administered sodium salicylate on biomarkers of pain in Holstein calves following castration and dehorning.Am J Vet Res 72 (2011): 1305-1317.
- Walsh SL, Chausmer AE, Strain EC, et al. Evaluation of the Mu and Kappa Opioid Actions of Butorphanol in Humans Through Differential Naltrexone Blockad. Psychopharmacology(Berl) 196 (2008): 143-155.
- Boas RA, Villiger JW. Clinical actions of fentanyl and buprenorphine. The significance of receptor binding. Br J Anaesth 57 (1985): 192-196.
- Dahan A, Yassen A, Bijl H, et al. Comparison of the respiratory effects of intravenous bupre-norphine and fentanyl in humans and rats.Br J Anaesth 94 (2005): 825-834.
- Talbert RL, Peters JI, Sorrells SC, et al. Respiratory effects of high-dose butorphanol. Acute Care 12 (1988): 47-56.
- Johnson JA, Robertson SA, Pypendop BH. Antinociceptive effects of butorphanol, bupre-norphine, or both, administered intramuscularly in cats. Am J Vet Res 68 (2007): 699-703.

 Impact Factor: * 1.1
Impact Factor: * 1.1 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 