Cutaneous Rosai-Dorfman Disease Showing Pruritic Macules
Article Information
Mayumi Ota, MD, Yoshimasa Nobeyama, MD*, and Akihiko Asahina, MD
Department of Dermatology, The Jikei University School of Medicine, Tokyo, Japan
*Corresponding Author: Yoshimasa Nobeyama, Department of Dermatology, The Jikei University School of Medicine, 25-8, Nishi-Shimbashi 3-chome, Minato-ku, Tokyo 105-8461, Japan
Received: 03 May 2021; Accepted: 14 May 2021; Published: 20 May 2021
Citation: Mayumi Ota, Yoshimasa Nobeyama, Akihiko Asahina. Cutaneous Rosai-Dorfman Disease Showing Pruritic Macules. Archives of Clinical and Medical Case Reports 5 (2021): 434-439.
View / Download Pdf Share at FacebookAbstract
Cutaneous Rosai-Dorfman disease (CRDD) is a rare skin-limited form of Rosai-Dorfman disease, a benign histiocytic proliferative disorder commonly affecting lymph nodes. Here, we report a case of CRDD characterized by pruritic reddish-brown macules, which we initially misdiagnosed as post-inflammatory pigmentation due to uremic dermatitis. A 64-year-old Japanese man was referred to us with an 8-month history of pruritic eruption located in the trunk and limbs. He had been receiving dialysis for chronic renal failure for 24 years. Physical examination revealed multiple reddish-brown macules measuring 1–10 cm in diameter with scratch marks irregularly distributed on the trunk and limbs. Pruritic score on the Numeric Rating Scale (NRS) was 9 out of 10. The patient displayed no extracutaneous involvements such as lymphadenopathy, fever or weight loss. Histopathological examination of the reddish-brown macules showed dense infiltration of histiocytes with lymphocytes and plasma cells in the dermis covered by epidermis with a faintly pigmented basal layer. Some histiocytes had taken in red blood cells, representing so-called emperipolesis. Immunohistochemical analyses of histiocytes showed reactivity to anti-S-100 protein antibodies and anti-CD68 antibodies, but not to anti-CD1a antibodies. Based on these findings, CRDD was diagnosed. This case suggests that CRDD may present with: i) macular lesions in the active phase; and ii) severe pruritus.
Keywords
Rosai-Dorfman disease; Pruritus; Macule; Emperipolesis; Histiocytosis
Article Details
1. Introduction
Rosai-Dorfman disease (RDD) is a rare, benign histiocytic proliferative disorder that frequently involves lymphadenopathy [1] and extranodal involvements such as pyrexia, polyclonal gammopathy and neutrophilia with a medium frequency. Indeed, Foucar et al. reported that the extranodal organs were affected in approximately 40% of cases, with the skin as one of the most commonly affected extranodal organs [2]. Cutaneous manifestations of RDD include papules, nodules, plaques, masses and ulcers, which may be located in any region [2-4]. Because of the wide variety of clinical manifestations, the diagnosis must be made based on histopathological and immunohistochemical findings of dense infiltration of histiocytes with positive reactivity to anti-S-100 protein along with anti-CD68 antibodies and negative reactivity to anti-CD1a antibodies [3-5]. The diagnosis is further confirmed through the detection of emperipolesis, representing histiocytes that have taken in lymphocytes, plasma cells, neutrophils and red blood cells.
Cutaneous RDD (CRDD) is a subtype of RDD in which the lesions are localized in skin tissue without any extracutaneous symptoms such as lymphadenopathy. This subtype accounts for only 3% of all RDD cases [6]. Here, we report a case of CRDD characterized by pruritic reddish-brown macules, which we initially misdiagnosed as post-inflammatory pigmentation due to uremic dermatitis.
2. Case Report
A 64-year-old Japanese man was referred to us with an 8-month history of pruritic eruption located in the trunk and limbs. The patient had been treated in another clinic with prednisolone at 0.5 mg/kg once or twice a week, nalfurafine hydrochloride at 2.5 µg/day, bepotastine besilate at 20 mg/day and topical betamethasone butyrate propionate, resulting in no response. He had been receiving dialysis for chronic renal failure for 24 years, and had undergone nephrectomy for left renal cell carcinoma 4 years before this presentation.
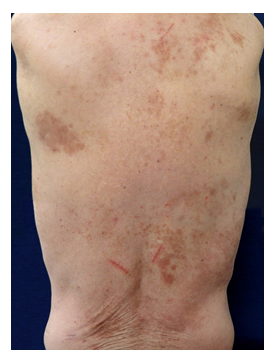
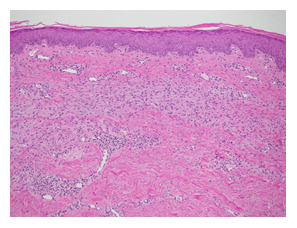
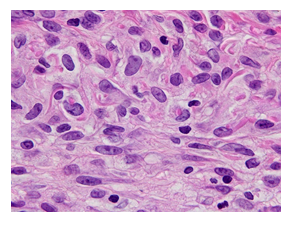
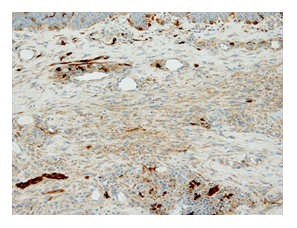
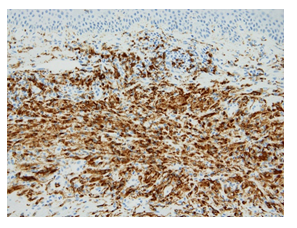
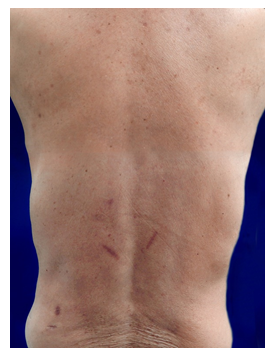
Physical examination revealed multiple reddish-brown macules measuring 1–10 cm in diameter with scratch marks irregularly distributed on the trunk and limbs (Figure 1). Pruritic score on the Numeric Rating Scale (NRS) was 9 out of 10. The patient displayed no extracutaneous involvements such as lymphadenopathy, fever or weight loss. Histopathological examination of the reddish-brown macules showed dense infiltration of histiocytes with lymphocytes and plasma cells in the dermis covered by epidermis with a faintly pigmented basal layer (Figure 2). Some histiocytes had taken in red blood cells, representing so-called emperipolesis (Figure 3). Immunohistochemical analyses of histiocytes showed reactivity to anti-S-100 protein antibodies (Agilent, Santa Clara, CA) and anti-CD68 antibodies (Agilent) (Figure 4 and 5), but not to anti-CD1a antibodies (Agilent). Based on these findings, CRDD was diagnosed. The patient was treated with prednisolone at 0.5 mg/kg/day and narrow-band ultraviolet B irradiation twice at a 2-week interval, and pruritic sensation was relieved (NRS, 0). Administration of prednisolone was ceased within 2 months after the first visit, by which time the eruptions had almost disappeared (Figure 6).
3. Discussion
Because CRDD occasionally shows spontaneous regression and usually presents with nodules or plaques as the clinical manifestation [7], the macular lesions on the first visit in our case might be considered as simply a clinical manifestation in the regression process from plaque or nodular lesions. However, our case was strongly suggested to have presented with macular lesions in the active phase of the disease, because: i) the patient had not noticed the appearance of nodular or plaque lesions during the course of the disease in situations where the patient would have looked at and touched the lesions located on the trunk and limbs due to severe pruritus; ii) histopathological examination of the macular lesions showed massive histiocytic infiltration and many instances of emperipolesis, which is found only in recently developed lesions, and not in older lesions [3]; and iii) eruptions had almost disappeared within 2 months, in contrast with the fact that post-inflammatory pigmentation is more persistent.
Previous reports have described the ineffectiveness of various treatments for CRDD, including topical and systemic corticosteroids, radiation therapy and phototherapy, although surgical excision appears effective for solitary lesion [8]. In this context, no therapeutic strategy has been established for CRDD showing multiple lesions. Principally, therapy for CRDD may not be needed, because: i) the prognosis is good and most cases will show spontaneous regression over a period of months to years; and ii) no cases of cutaneous disease progressing to systemic disease have been reported [2,5]. However, our patient was in exceptional need of treatment because of the severe pruritus. Immediately after performing narrow-band ultraviolet B irradiation in combination with administering a medium dose of systemic corticosteroid in addition to an anti-histamine and a topical corticosteroid, the patient was very satisfied with the decrease in the pruritic sensation. We still lack evidence that narrow-band ultraviolet B irradiation in combination with systemic corticosteroid administration is effective against CRDD, considering that the disease can regress spontaneously.
In conclusion, CRDD may present with macular lesions in the active phase and severe pruritus. Further study is required to elucidate the clinical manifestations and pathogenesis of this disease.
References
- Rosai J, Dorfman RF. Sinus histiocytosis with massive lymphadenopathy. A newly recognized benign clinicopathological entity. Arch Pathol 87 (1969): 63-70.
- Foucar E, Rosai J, Dorfman R. Sinus histiocytosis with massive lymphadenopathy (Rosai-Dorfman disease): review of the entity. Semin Diagn Pathol 7 (1990): 19-73.
- Gameiro A, Gouveia M, Cardoso JC, et al. Histological variability and the importance of clinicopathological correlation in cutaneous Rosai-Dorfman disease. An Bras Dermatol 91 (2016): 634-637.
- Rubenstein MA, Farnsworth NN, Pielop JA, et al. Cutaneous Rosai-Dorfman disease. Dermatol Online J 12 (2006): 8.
- Brenn T, Calonje E, Granter SR, et al. Cutaneous rosai-dorfman disease is a distinct clinical entity. Am J Dermatopathol 24 (2002): 385-391.
- Wang KH, Chen WY, Liu HN, et al. Cutaneous Rosai-Dorfman disease: clinicopathological profiles, spectrum and evolution of 21 lesions in six patients. Br J Dermatol 154 (2006): 277-286.
- Kroumpouzos G, Demierre MF. Cutaneous Rosai-Dorfman disease: histopathological presentation as inflammatory pseudotumor. A literature review. Acta Derm Venereol 82 (2002): 292-296.
- Kong YY, Kong JC, Shi DR, et al. Cutaneous rosai-dorfman disease: a clinical and histopathologic study of 25 cases in China. Am J Surg Pathol 31 (2007): 341-350.


 Impact Factor: * 3.1
Impact Factor: * 3.1 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 
