Extraforaminal Lumbar Disc Herniation-How to Approach
Article Information
Inaki Arrotegui*
Department of Neurosurgery, University General Hospital of Valencia, Valencia, Spain
*Corresponding Author: Inaki Arrotegui, Department of Neurosurgery, University General Hospital of Valencia, Avda Tres Cruces S/n. 46014-Valencia, Spain.
Received: 23 May 2019; Accepted: 04 June 2019; Published: 17 June 2019
Citation:
Inaki Arrotegui. Extraforaminal Lumbar Disc Herniation-How to Approach. Journal of Spine Research and Surgery 1 (2019): 033-036.
View / Download Pdf Share at FacebookKeywords
Herniated discs, Spinal canal, Herniation, Treatment
Herniated discs articles Herniated discs Research articles Herniated discs review articles Herniated discs PubMed articles Herniated discs PubMed Central articles Herniated discs 2023 articles Herniated discs 2024 articles Herniated discs Scopus articles Herniated discs impact factor journals Herniated discs Scopus journals Herniated discs PubMed journals Herniated discs medical journals Herniated discs free journals Herniated discs best journals Herniated discs top journals Herniated discs free medical journals Herniated discs famous journals Herniated discs Google Scholar indexed journals Spinal canal articles Spinal canal Research articles Spinal canal review articles Spinal canal PubMed articles Spinal canal PubMed Central articles Spinal canal 2023 articles Spinal canal 2024 articles Spinal canal Scopus articles Spinal canal impact factor journals Spinal canal Scopus journals Spinal canal PubMed journals Spinal canal medical journals Spinal canal free journals Spinal canal best journals Spinal canal top journals Spinal canal free medical journals Spinal canal famous journals Spinal canal Google Scholar indexed journals Herniation articles Herniation Research articles Herniation review articles Herniation PubMed articles Herniation PubMed Central articles Herniation 2023 articles Herniation 2024 articles Herniation Scopus articles Herniation impact factor journals Herniation Scopus journals Herniation PubMed journals Herniation medical journals Herniation free journals Herniation best journals Herniation top journals Herniation free medical journals Herniation famous journals Herniation Google Scholar indexed journals Treatment articles Treatment Research articles Treatment review articles Treatment PubMed articles Treatment PubMed Central articles Treatment 2023 articles Treatment 2024 articles Treatment Scopus articles Treatment impact factor journals Treatment Scopus journals Treatment PubMed journals Treatment medical journals Treatment free journals Treatment best journals Treatment top journals Treatment free medical journals Treatment famous journals Treatment Google Scholar indexed journals disc at lumbar articles disc at lumbar Research articles disc at lumbar review articles disc at lumbar PubMed articles disc at lumbar PubMed Central articles disc at lumbar 2023 articles disc at lumbar 2024 articles disc at lumbar Scopus articles disc at lumbar impact factor journals disc at lumbar Scopus journals disc at lumbar PubMed journals disc at lumbar medical journals disc at lumbar free journals disc at lumbar best journals disc at lumbar top journals disc at lumbar free medical journals disc at lumbar famous journals disc at lumbar Google Scholar indexed journals subarticular hernias articles subarticular hernias Research articles subarticular hernias review articles subarticular hernias PubMed articles subarticular hernias PubMed Central articles subarticular hernias 2023 articles subarticular hernias 2024 articles subarticular hernias Scopus articles subarticular hernias impact factor journals subarticular hernias Scopus journals subarticular hernias PubMed journals subarticular hernias medical journals subarticular hernias free journals subarticular hernias best journals subarticular hernias top journals subarticular hernias free medical journals subarticular hernias famous journals subarticular hernias Google Scholar indexed journals L4-L5 articles L4-L5 Research articles L4-L5 review articles L4-L5 PubMed articles L4-L5 PubMed Central articles L4-L5 2023 articles L4-L5 2024 articles L4-L5 Scopus articles L4-L5 impact factor journals L4-L5 Scopus journals L4-L5 PubMed journals L4-L5 medical journals L4-L5 free journals L4-L5 best journals L4-L5 top journals L4-L5 free medical journals L4-L5 famous journals L4-L5 Google Scholar indexed journals neuropathic pain articles neuropathic pain Research articles neuropathic pain review articles neuropathic pain PubMed articles neuropathic pain PubMed Central articles neuropathic pain 2023 articles neuropathic pain 2024 articles neuropathic pain Scopus articles neuropathic pain impact factor journals neuropathic pain Scopus journals neuropathic pain PubMed journals neuropathic pain medical journals neuropathic pain free journals neuropathic pain best journals neuropathic pain top journals neuropathic pain free medical journals neuropathic pain famous journals neuropathic pain Google Scholar indexed journals posterolateral herniations articles posterolateral herniations Research articles posterolateral herniations review articles posterolateral herniations PubMed articles posterolateral herniations PubMed Central articles posterolateral herniations 2023 articles posterolateral herniations 2024 articles posterolateral herniations Scopus articles posterolateral herniations impact factor journals posterolateral herniations Scopus journals posterolateral herniations PubMed journals posterolateral herniations medical journals posterolateral herniations free journals posterolateral herniations best journals posterolateral herniations top journals posterolateral herniations free medical journals posterolateral herniations famous journals posterolateral herniations Google Scholar indexed journals
Article Details
1. Introduction
Not all herniated discs are the same or require the same type of treatment or the same surgical approach. The most common location of a herniated disc is the inside of the spinal canal. In the following sample of magnetic resonances we can observe the different locations of the herniated discs with respect to the spinal canal (Figure 1).
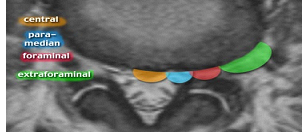
Figure 1: Location of the different types of disc at lumbar level.
Probably, the most surgical disc are the subarticular hernias, which involve the nerve just before its exit by the lateral recess of the canal. But the foraminal (Figure 2) and extraforaminal (Figure 3) hernias are a little special case due to several circumstances. In the first place they are very infrequent. They probably represent less than 10% of herniated discs. They are named after their close relationship with the neural foramen, a grossly tubular space through which the nerve root leaves the neural canal to the soft tissues to form the lumbosacral plexus and subsequently the sciatic trunk.
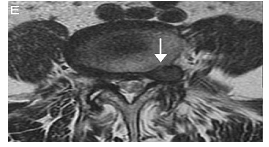
Figure 2: Lumbar disc Herniation at Foraminal space.
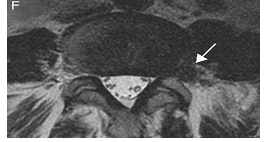
Figure 3: Lumbar herniation at extraforaminal space.
They are also a special case because they affect the outgoing root instead of the descending root. For example, in the typical case of level L4-L5, the root affected by a herniated canal is L5, in its descending course towards the next foramen, while both a foraminal and an extraforaminal hernia, will affect the L4 root, with a different pain distribution. Regarding their prognosis and treatment, these types of hernias also have a different behavior than other common hernias. Unless they are very bulky hernias that cause paralysis or discs extremely disabling pain, with enough patience, most of these cases are resolved without surgery. With adequate treatment, it is likely that within 3 months the pain has disappeared or is very tolerable.
The surgery is also different in these cases, since the traditional approaches through the canal do not allow to visually control the lesion and its extirpation. When surgery is necessary, access is not made through the midline of the back, but slightly lateralized through the musculature, to directly access the foramen. This type of approach has its implications, since it leads directly to a very sensitive part of the nerve that is the neural ganglion. The excessive manipulation of the ganglion, sometimes necessary for the detachment of the hernia, can cause loss of sensitivity or discomfort (neuropathic pain) in some cutaneous area. Therefore, it is highly recommended to try conservative treatment before venturing into surgery.
2. A case
The patient had as its main symptom radicular pain, to the examination physical presented paresis and, sensitive alteration in the root territory committed in the affected lower extremity. The diagnosis The definitive study was based on the study of images with computed tomography and/or resonance. Level affected corresponded to L4-L5. The patient received conservative treatment with rest and non-steroidal anti-inflammatory drugs in the preoperative period.
3. Discussion
The extraforaminal herniation, understood like those herniated discs that compress the root outside the limits bone of the conjunction hole, constitute a variable percentage of agreement to the different series, representing between 0.7-12% of all lumbar discs [1, 2]. It affects men and women alike, in the middle age of life, between 50-78 years1. Unlike the posterolateral herniations are presented predominantly at levels L3-L4 and L4-L5, followed by L5-S11 [3]. Extraforaminal discs, described for the first time by Abdullah et al, in 19744, correspond to a percentage minor, but not negligible of all Lumbar herniated discs [4]. They require a special surgical approach, which poses a challenge for the surgeon accustomed to the interlaminar approach [5, 6]. There are several techniques described. The most common approach via posteromedial with hemilaminectomy and facetectomy complete or partial, offers a known way of access and a good visualization of the committed root, but at generate a wide joint resection, can lead to later problems of instability of the spine, and pain lumbar [7-9]. The clinical syndrome that they generate produced by nerve compression and ganglion that emerge in the same level. This is how in a herniated disc extraforaminal L3-L4 is affected root L3, at level L4-L5 the root L4, at level L5-S1 the root will be affected L5 In general, they present with pain radicular and neurological deficit, either motor or sensitive in more than 75% of cases [10, 11]. With regard to their treatment, patients can initially submit to a conservative management, with rest, analgesics and anti-inflammatories, which succeeds in a low percentage of the cases3. That is why the treatment Surgical is usually necessary. He has described several surgical techniques, with particular advantages and disadvantages that do not exist consensus in which one is the best. We can mention: Laminectomy with total facetectomy or partial, transverse approach, paramedial extraforaminal, retroperitoneal anterolateral, intertransverse boarding and more recently endoscopic techniques minimally invasive [12, 13].
4. Conclusion
The technique presented in this report, consists of a medium-line approach with dissection and retraction of the musculature paraspinal, exposure of intertransverse space, identification and resection of the intertransverse membrane, identification of the nerve root and your ganglion, and scan under them to identify and resect the disc fragment herniated, with eventual discectomy.
References
- Epstein NE. Foraminal and far lateral lumbar disc herniations: surgical alternatives and outcome measures. Spinal Cord 40 (2002): 491-500.
- Porchet F. Long-term follow up of patients surgically treated by the far-lateral approach for foraminal and extraforaminal lumbar disc herniations J Neurosurgery Spine 90 (1999): 59-66.
- Epstein NE. Different surgical approaches to far lateral lumbar disc herniations. J Spinal Disord 8 (1995): 383-394.
- Abdullah AF, Ditto EW III, Byrd EB, et al. Extremelateral lumbar disk herniations. Clinical syndrome and special problems of diagnosis. J Neurosurg 41 (1974): 229-234.
- Quaglietta P. Paraspinal approach to the far lateral disc herniations: retrospective study on 42 cases. Acta Neurochir 92 (2005): 115-119.
- Abdullah AF, Wolber PGH, Warfield JR, et al. Surgical management of extreme lateral lumbar disc herniations: review of 138 cases. Neurosurgery 22 (1988): 648-653.
- Garrido E, Connaughton PN. Unilateral facetectomy approach for lateral lumbar disc herniation. J Neurosurg 74 (1991): 754-756.
- Glenn Richard. Atlas of neurosurgical techniques. Spine and peripheral nerves. Far lateral microdiskectomy (Emily Friedman Chapter 87 (2006): 638-643.
- Khalil Salame, Zvi Lidar. Minimally invasive approach to far lateral lumbar disc herniation: technique and clinical results. Acta Neurochir 152 (2010): 663-668.
- O’hara LJ, Marshall RW. Far lateral lumbar disc herniation: the key to the intertransverse approach. The journal of bone and joint surgery 79 (1997).
- Mehmet Faik Ozveren. Combined approach for far lateral lumbar disc herniation. Neurol Med Chir (Tokio) 44 (2004): 118-123.
- Ricky Madhok MD, and Adam S. Kanter, MD, Extreme-lateral, minimally invasive, transpsoas approach for the treatment of far-lateral lumbar disc herniation, J Neurosurg Spine 2010; 12: 347-350.
- Stephen M Pirris, Sanjay Dhall, Praveen V Mummaneni, et al. Minimally invasive approach to extraforaminal disc herniations at the lumbosacral junction using an operating microscope: case series and review of the literature. Neurosurg Focus 25 (2008): 10.


 Impact Factor: * 3.123
Impact Factor: * 3.123 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 14.90%
Acceptance Rate: 14.90%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 