Transverse Testicular Ectopia: A Rare Diagnosis during Herniotomy
Article Information
Ismail AS Burud*, Farren Yeoh BH, Davaraj Balasingh KP Sundram
Department of General Surgery, Clinical Campus, International Medical University, Seremban, Malaysia
*Corresponding Author: Ismail AS Burud, Department of General Surgery, Clinical Campus, International Medical University, Seremban, Malaysia
Received: 16 January 2019; Accepted: 28 January 2019; Published: 02 February 2019
Citation: Ismail AS Burud, Farren Yeoh BH, Davaraj Balasingh KP Sundram. Transverse Testicular Ectopia: A Rare Diagnosis during Herniotomy. Journal of Surgery and Research 2 (2019): 15-19.
View / Download Pdf Share at FacebookAbstract
Transverse testicular ectopia (TTE) is a condition characterized by migration of both testes towards the same hemiscrotum. The mean age of presentation is 4 years, with a typical presentation of a symptomatic inguinal hernia with contralateral impalpable testis. There is no reported predisposition to either left or right side. The diagnosis is usually intraoperative however, imaging modalities and diagnostic laparoscopy are useful in aiding pre-operative diagnosis. We present a case of a 5-year-old boy with a history of a painful swelling in the left inguinal region, with palpable left testis and contralateral empty scrotum. During the planned herniotomy in view of his pain, he was diagnosed with transverse testicular ectopia intra-operatively. Herniotomy on the left side with left testicular orchiopexy and transseptal fixation for the right testis was performed. He recovered well in the post-operative period. This rare congenital anomaly is often diagnosed intraoperatively as an incidental finding, and long-term follow up would be required due to the risk of malignant transformation.
Keywords
Hernia, Orchiopexy, Testicular ectopia, Undescended testes
Hernia articles Hernia Research articles Hernia review articles Hernia PubMed articles Hernia PubMed Central articles Hernia 2023 articles Hernia 2024 articles Hernia Scopus articles Hernia impact factor journals Hernia Scopus journals Hernia PubMed journals Hernia medical journals Hernia free journals Hernia best journals Hernia top journals Hernia free medical journals Hernia famous journals Hernia Google Scholar indexed journals Orchiopexy articles Orchiopexy Research articles Orchiopexy review articles Orchiopexy PubMed articles Orchiopexy PubMed Central articles Orchiopexy 2023 articles Orchiopexy 2024 articles Orchiopexy Scopus articles Orchiopexy impact factor journals Orchiopexy Scopus journals Orchiopexy PubMed journals Orchiopexy medical journals Orchiopexy free journals Orchiopexy best journals Orchiopexy top journals Orchiopexy free medical journals Orchiopexy famous journals Orchiopexy Google Scholar indexed journals Testicular ectopia articles Testicular ectopia Research articles Testicular ectopia review articles Testicular ectopia PubMed articles Testicular ectopia PubMed Central articles Testicular ectopia 2023 articles Testicular ectopia 2024 articles Testicular ectopia Scopus articles Testicular ectopia impact factor journals Testicular ectopia Scopus journals Testicular ectopia PubMed journals Testicular ectopia medical journals Testicular ectopia free journals Testicular ectopia best journals Testicular ectopia top journals Testicular ectopia free medical journals Testicular ectopia famous journals Testicular ectopia Google Scholar indexed journals Undescended testes articles Undescended testes Research articles Undescended testes review articles Undescended testes PubMed articles Undescended testes PubMed Central articles Undescended testes 2023 articles Undescended testes 2024 articles Undescended testes Scopus articles Undescended testes impact factor journals Undescended testes Scopus journals Undescended testes PubMed journals Undescended testes medical journals Undescended testes free journals Undescended testes best journals Undescended testes top journals Undescended testes free medical journals Undescended testes famous journals Undescended testes Google Scholar indexed journals Transverse testicular ectopia articles Transverse testicular ectopia Research articles Transverse testicular ectopia review articles Transverse testicular ectopia PubMed articles Transverse testicular ectopia PubMed Central articles Transverse testicular ectopia 2023 articles Transverse testicular ectopia 2024 articles Transverse testicular ectopia Scopus articles Transverse testicular ectopia impact factor journals Transverse testicular ectopia Scopus journals Transverse testicular ectopia PubMed journals Transverse testicular ectopia medical journals Transverse testicular ectopia free journals Transverse testicular ectopia best journals Transverse testicular ectopia top journals Transverse testicular ectopia free medical journals Transverse testicular ectopia famous journals Transverse testicular ectopia Google Scholar indexed journals pre-operative diagnosis articles pre-operative diagnosis Research articles pre-operative diagnosis review articles pre-operative diagnosis PubMed articles pre-operative diagnosis PubMed Central articles pre-operative diagnosis 2023 articles pre-operative diagnosis 2024 articles pre-operative diagnosis Scopus articles pre-operative diagnosis impact factor journals pre-operative diagnosis Scopus journals pre-operative diagnosis PubMed journals pre-operative diagnosis medical journals pre-operative diagnosis free journals pre-operative diagnosis best journals pre-operative diagnosis top journals pre-operative diagnosis free medical journals pre-operative diagnosis famous journals pre-operative diagnosis Google Scholar indexed journals testicular orchiopexy articles testicular orchiopexy Research articles testicular orchiopexy review articles testicular orchiopexy PubMed articles testicular orchiopexy PubMed Central articles testicular orchiopexy 2023 articles testicular orchiopexy 2024 articles testicular orchiopexy Scopus articles testicular orchiopexy impact factor journals testicular orchiopexy Scopus journals testicular orchiopexy PubMed journals testicular orchiopexy medical journals testicular orchiopexy free journals testicular orchiopexy best journals testicular orchiopexy top journals testicular orchiopexy free medical journals testicular orchiopexy famous journals testicular orchiopexy Google Scholar indexed journals transseptal fixation articles transseptal fixation Research articles transseptal fixation review articles transseptal fixation PubMed articles transseptal fixation PubMed Central articles transseptal fixation 2023 articles transseptal fixation 2024 articles transseptal fixation Scopus articles transseptal fixation impact factor journals transseptal fixation Scopus journals transseptal fixation PubMed journals transseptal fixation medical journals transseptal fixation free journals transseptal fixation best journals transseptal fixation top journals transseptal fixation free medical journals transseptal fixation famous journals transseptal fixation Google Scholar indexed journals retroperitoneal testis articles retroperitoneal testis Research articles retroperitoneal testis review articles retroperitoneal testis PubMed articles retroperitoneal testis PubMed Central articles retroperitoneal testis 2023 articles retroperitoneal testis 2024 articles retroperitoneal testis Scopus articles retroperitoneal testis impact factor journals retroperitoneal testis Scopus journals retroperitoneal testis PubMed journals retroperitoneal testis medical journals retroperitoneal testis free journals retroperitoneal testis best journals retroperitoneal testis top journals retroperitoneal testis free medical journals retroperitoneal testis famous journals retroperitoneal testis Google Scholar indexed journals transseptal orchiopexy articles transseptal orchiopexy Research articles transseptal orchiopexy review articles transseptal orchiopexy PubMed articles transseptal orchiopexy PubMed Central articles transseptal orchiopexy 2023 articles transseptal orchiopexy 2024 articles transseptal orchiopexy Scopus articles transseptal orchiopexy impact factor journals transseptal orchiopexy Scopus journals transseptal orchiopexy PubMed journals transseptal orchiopexy medical journals transseptal orchiopexy free journals transseptal orchiopexy best journals transseptal orchiopexy top journals transseptal orchiopexy free medical journals transseptal orchiopexy famous journals transseptal orchiopexy Google Scholar indexed journals
Article Details
1. Introduction
Transverse testicular ectopia (TTE) is a rare congenital anomaly where both testes migrates ipsilaterally towards the same hemiscrotum while the contralateral inguinal canal and hemiscrotum is empty. It was first reported by Von Lenhossek in 1886 as an autopsy finding [1]. Presentation is usually that of an inguinal hernia with ipsilateral palpable testis and an impalpable testis on the other side. Occasionally, two globular structures are palpable on the hernia side [2]. The classical description of TTE consists of two testes that are found on one side of the body while it is absent on the other side. They are identical in size and appearance, each with its own individual separate epididymis, vas deferens and testicular vessels. The vascular supply and the vas deferens of the ectopic testis is from the appropriate side. On the side of the two testes, the processus vaginalis is patent while conversely, there is no hernia on the contralateral side [3]. The diagnosis of TTE is usually made intraoperatively as surgery is indicated for hernia and the rarity of TTE eludes a pre-operative diagnosis.
2. Case Presentation
A 5-year-old boy was referred by a general practitioner to the surgical outpatient department with history of a painful swelling in the left inguinal region since infancy. There were no other complains related to this swelling. His younger brother was healthy and had no complaints. On examination of the inguinal region and the scrotum, there was positive cough impulse on the left side and the swelling was reducible. The left testis was palpable. The right side of the scrotum was underdeveloped and the testis was absent. Cough impulse on the right side was absent. With a clinical diagnosis of left inguinal hernia with right undescended testis, he was posted for a herniotomy in view of his pain. Intraoperatively, the hernia sac was identified and both testes unexpectedly delivered from the incisional wound. Each testis appeared normal with separate epididymis, vas deferens and testicular vessels (Figure 1). Both spermatic cords followed the left deep inguinal ring and entered the abdomen. The hernial sac was separated carefully and a herniotomy was performed. The left testis was secured in the left hemiscrotum. The right testis was fixed at the right subdartos pouch through the transseptal window using Vicryl 4/0 (Figure 2). There were no complications in the postoperative period and he was well on discharge. Ultrasound of the abdomen and pelvis done during the follow-up was normal.
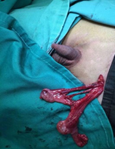
Figure 1: Both Testis with separate cord structures.
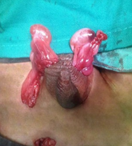
Figure 2: Both Testis fixed in each side of the scrotum.
3. Discussion
In utero, the descent of the retroperitoneal testis from the lumbar area (ventro-medial to the atrophied mesonephros) to the scrotum is attributed to the shortening of the gubernaculum. Cryptorchidism is defined as the failure of a testis to descend into its scrotal position, and this can be divided into acquired or congenital. Congenital cryptorchidism can be classified into either true undescended testes or ectopic testes. An ectopic testis descends through the external ring normally but is then diverted to an aberrant position. Testes that are situated in the superficial inguinal pouch are classified as ectopic but they should be considered as a variant of undescended testes [4]. Amongst the variants of ectopic testes, perineal ectopic testis is the most common. Other reported variants are femoral ectopic testis, pubopenile ectopic testis and TTE. TTE occurs when both testes migrate through a single inguinal canal towards a common hemiscrotum. Besides TTE, the terms “transverse abberant testicular maldescent, testicular pseudoduplication, and unilateral double testes” has been used in the literature to describe this similar condition [5]. Theories explaining the pathology of TTE include both testes being derived from the same germinal ridge, mechanical effect of persistent Mullerian duct structures preventing testicular descent or causing both testes to descend towards the same hemiscrotum, and defective gubernacular formation [6]. TTE is classified into three types according to the associated anomalies:
Type I: associated to inguinal hernia alone.
Type II: associated to persistent Mullerian remnants.
Type III: associated to other anomalies other than Mullerian remnants [2].
Persistent Mullerian duct syndrome with TTE has been reported in 20% to 49% of the cases [7]. Besides persistent Mullerian remnants, other associated anomalies that had been reported includes common vas deferens, seminal vesicle cyst and bilateral renal dysgenesis [5]. The ectopic testis carries an increased risk of infertility and a 5-10-fold increased lifetime risk of testicular neoplasia. It is typically characterized by a significant lack of germ cells, consequently infertility can often persist, even after early surgical intervention. It is interesting to note that there appears to be no impact on the testosterone levels despite the significant negative effect on fertility. Hence, the primary objective of early surgical management is to reduce the risk of testicular neoplasia as well as for cosmetic purposes [6].
Although most cases of TTE are diagnosed intra-operatively during a surgery for hernia or exploration for an undescended testis, pre-operative investigations such as ultrasonography (US), magnetic resonance imaging (MRI), arteriography, venography, computed topography [8] and diagnostic laparoscopy has been described to aid in the diagnosis. A pre-operative diagnosis allows assessment of the length of the spermatic vessels and the anatomy of the two vasa deferentia before committing to a particular mode of orchiopexy [7]. Arteriography and venography are invasive and requires general anaesthesia, a factor that needs to be taken into consideration when performed on paediatric patients. US has a sensitivity ranging from 82 to 88% in the detection of an impalpable testis [8]. A diagnostic laparoscopy has an additional benefit of allowing concurrent biopsies of gonads and Mullerian duct remnants to be taken [7]. Magnetic resonance venography (MRV) has a sensitivity of 100% with the main objective of localising the testicular vessels instead of imaging the testicular tissue. An approach in the work-up of the impalpable testis recommended by Lam et. al involves performing US as a first-line imaging modality due to its easy availability and lack of ionising radiation. If US findings are negative, MRI (which has a comparable sensitivity of 84%) is recommended as the next line of investigation, followed by MRV as the third line of investigation [8].
The main outline of the surgical management consists of fixation of the testes into the scrotum, searching for Mullerian duct remnants and other anomalies and long-term follow up to monitor for malignant changes. Surgical fixation can be accomplished by either a transseptal orchiopexy or extraperitoneal transposition of the testis. As Mullerian duct remnants rarely undergoes malignant degeneration, they should be managed conservatively if they are encountered intra-operatively. However, there had been reported cases of malignant degeneration of Mullerian duct remnants [9, 10]. If the decision was made to remove the Mullerian duct remnants, extra precaution should be taken to ensure there is no vascular compromise of the vas deferens, which has a blood supply closely related to Mullerian derivatives. Apart from an open approach, either a fully laparoscopic approach or a laparoscopic-aided surgery had been reported to be successful in the management of TTE [7].
4. Conclusion
TTE is a rare congenital anomaly which should be suspected in a child during the clinical evaluation of an inguinal hernia with contralateral impalpable testis, as demonstrated in our case. TTE cases are incidental intra-operative findings during herniotomy. Surgical management which includes transseptal orchiopexy is indicated expediently to reduce the risk of testicular malignant changes, with long-term follow-up to monitor for such transformation.
Acknowledgements
We would like to acknowledge and thank the Director General of Health Malaysia for granting us the permission to publish this case report. This case report has been approved and registered at the National Medical Research Register Secretariat, Malaysia with the ID as mentioned NMRR ID: NMRR-18-226-40237.
Conflict of Interest
The author(s) declared no potential conflicts of interest nor any funding involved in the publication of the article.
References
- Von Lenhossek MN. Ectopia testis transversa. Anat Anz 1 (1886): 376-381.
- Esteves E, Pinus J, Maranhao RF, et al. Crossed testicular ectopia. Sao Paulo Med J 113 (1995): 935-940.
- De Luna AM, Ortenberg J, Craver RD. Exploration for testicular remnants: Implications of residual seminiferous tubules and crossed testicular ectopia. J Urol 169 (2003): 1486-1489.
- Murphy DM, Butler MR. Preperitoneal ectopic testis: A case report. J Pediatr Surg 20 (1985): 93-94.
- Naji H, Peristeris A, Stenman J, et al. Transverse testicular ectopia: Three additional cases and a review of the literature. Pediatr Surg Int 28 (2012 ): 703-706.
- Punwani VV, Wong JSY, Lai CYH, et al. Testicular ectopia: Why does it happen and what do we do? J Pediatr Surg 52 (2017): 1842-1847.
- Deshpande AV, La Hei ER. Impact of laparoscopy on the management of transverse testicular ectopia. J Laparoendosc Adv Surg Tech A 19 (2009): 443-446.
- Lam WW, Le SD, Chan KL, et al. Transverse testicular ectopia detected by MR imaging and MR venography. Pediatr Radiol 32 (2002): 126-129.
- Thiel DD, Erhard MJ. Uterine adenosarcoma in a boy with persistent müllerian duct syndrome: First reported case. J Pediatr Surg 40 (2005): 29-31.
- Shinmura Y, Yokoi T, Tsutsui Y. A case of clear cell adenocarcinoma of the müllerian duct in persistent mullerian duct syndrome: The first reported case. Am J Surg Pathol 26 (2002): 1231-1234.


 Impact Factor: * 4.2
Impact Factor: * 4.2 CiteScore: 2.9
CiteScore: 2.9  Acceptance Rate: 11.01%
Acceptance Rate: 11.01%  Time to first decision: 10.4 days
Time to first decision: 10.4 days  Time from article received to acceptance: 2-3 weeks
Time from article received to acceptance: 2-3 weeks 